HMO Enrollment Part 2 Focus on Commercial Plans
February 2, 2002
In an earlier Trend Note, we noted the general downward enrollment trend faced by HMOs in the states that we study. Some readers wrote in to point out the specific issues faced by commercial plans, and we want to add some information about them. Our recently released reports on managed care in Florida and Michigan provide vivid illustrations of what is happening.Faced with rising health care costs, employers turned to HMOs in significant numbers in the early 1990s. Enrollment in commercial HMO plans grew steadily, as employers left indemnity plans and lightly managed PPOs. To meet the new demand, national insurance carriers stepped up their marketing of HMO plans that offered broad provider networks. And to compete, many of the classic HMOs began to expand their networks through contracts with independent clinics.
During the mid-1990s, premium rates for commercial plans rose only a little, for several reasons. There was aggressive pricing by new start-up plans trying to gain market share and matched by the existing plans. Also, medical inflation was lower, as pharmaceutical companies and others tried to keep a low profile during the Clinton health plan debate.
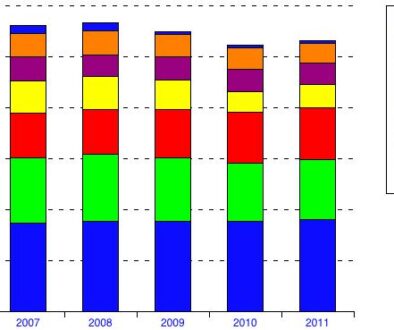
But a few years later, premium rates began to grow rapidly. HMOs were no longer willing to take market share over profitability and starting raising their prices. Medical inflation grew sharply because of pharmaceuticals and because hospital systems had gained leverage in their price negotiations with health plans. State regulation and public opinion pressed health plans to back away from aggressive medical management and generally made it more difficult to operate a commercial HMO. The chart below shows the rise and fall of commercial HMO enrollment for seven states.
For example, enrollment in commercials HMOs in Florida peaked at 3.7 million in 1999. It fell by 80,000 lives in 2000 and by another 134,000 lives in the first half of 2001. Over those 18 months, commercial enrollment fell by 5.8%. For additional information about Florida Managed Care Review 2001, go to:Â https://allanbaumgarten.com/cfusion/fl_report.cfm
In Michigan, enrollment in commercial HMO plans peaked in 2000 at 2 million. But membership fell in the first three quarters of 2001. By the end of September, enrollment was down by 40,000 members, or a 2% decrease. For more information about Michigan Managed Care Review 2001, go to:Â https://allanbaumgarten.com/cfusion/mi_report.cfm
Where are the enrollees going? Anecdotal evidence suggests that most are going to PPOs and other less heavily regulated managed care plans. Note that the employer may continue to buy benefits through the same company, since plans like United HealthCare and Aetna are marketing a wide portfolio of arrangements. The PPO arrangements, especially for self-insured employers, offers the employers more flexibility in designing benefit plans since they are subject to fewer state requirements for mandated benefits. They can also add enrollee cost-sharing that is not always possible under state HMO laws, thus making them competitive on price with HMOs.