HMO Profitability and Premiums Rise in 2001-2002
June 17, 2003
Copyright ©2003 Allan Baumgarten 11This Trend Note looks at key financial indicators for HMOs: premium revenue trend, medical spending trend, the spread between them and profitability. The analysis is based on our research to prepare annual Managed Care Reviews in eight states: California, Colorado, Florida, Illinois, Michigan, Minnesota, Ohio and Texas. In 2003, we plan to publish a new report analyzing market issues in Wisconsin.
After years of losses for the HMO industry, HMOs generally regained profitability in 2001 and 2002. Their improved bottom line resulted largely from two factors: (1) successive years of HMOs increasing their premiums at double digit rates and (2) in a strategy that may seem counterintuitive, cutting back on their commercial enrollment. But even as their premiums increase, the HMOs are having difficulty staying ahead of increases in medical expenses and that portends future difficulties for the industry.
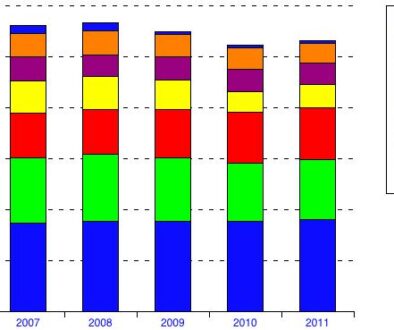
Exhibit 1 shows the growth of premium revenues for commercial HMOs in eight states. In the mid-1990s, HMO premium trend was low for several years. From 1994 to 1996, for example, Minnesota HMOs collected an average of $118 or so per member per month (PMPM) on their commercial enrollees, which put those HMOs in the middle of this group of states. In some states, the average PMPM actually decreased for one or two years.
Exhibit 1: HMO Average Commercial Premium Revenues Per Member Per Month, 1994-2002

Premiums stayed low for several reasons. First many local markets were hotly competitive because many new HMOs were created during that time. In Texas, for example, 20 new HMOs were licensed in 1996 and 1997. Ohio and Illinois also saw many new HMOs licensed then, although a few of them were never active. Both the startups and the established plans priced themselves aggressively to gain or maintain market share.
Second, HMOs were enjoying profits on their Medicare and Medicaid plans and sometimes used those surplus dollars to hold down commercial premium increases. Third, the use of capitation grew during this period, especially in markets where Medicare+Choice plans were prospering. Because HMOs were moving risk to provider groups, the HMOs felt less pressure to increase premiums even as it became apparent that medical costs were again on the rise. Finally, premiums may have been held down by the “Hillary effect,” when the national debates on health reform caused the health plans and pharmaceutical companies to keep a low profile and hold down their price increases.
The low premium trend of the mid-1990s was good news for employers, but was soon followed by years of large losses for HMOs. From 1997 to 2001, HMOs in Texas lost $1.5 billion. HMOs in other states did not fare as poorly but, as shown in Exhibit 2, HMOs in four of the other states lost money in 1999 and 2000. HMOs in Texas and Florida were still losing money in 2001.

Statewide numbers may be tilted in one direction or another by the results for one or two large plans. In Illinois, for example, HMO Illinois (part of Blue Cross Blue Shield of Illinois) has been consistently profitable. In 1999, HMO Illinois made $57.3 million. All the other HMOs in the state combined had a net loss of $21 million. But the bottom line for the industry shows up as positive net income of $36.4 million.
To stem their losses, HMOs did several things. First they raised their commercial premiums as much as local markets would bear. In 2001, average premium revenue increases ranged from 9.7% in Illinois to 18.5% in Texas. In Minnesota, premium revenues increased at double-digit rates for four straight years. Many that were losing money on their Medicare+Choice plans either ended those plans, cut back on service areas, or reduced supplemental benefits and increased enrollee co-premiums.
A second way in which HMOs cut their losses was by dropping unprofitable groups or converting them to self-funded plans. In the 18 months from December 2000 to June 2002, commercial HMO enrollment declined sharply in all of these states, ranging from 875,000 lives in Texas to 21,000 in Minnesota. (Minnesota HMOs lost many commercial enrollees prior to 2000.) On average, HMOs in these states lost 17% of their commercial members, a decrease of nearly 2.6 million lives. (For more details, see our earlier Trend Note, https://allanbaumgarten.com/cfusion/view_news.cfm?id=39 )
For example, United HealthCares commercial enrollment in Texas declined by 114,000 members, or 33.5% in that same 18-month period and it lost 103,000 commercial members from its Ohio HMO. According to United HealthCare sources, many of those employer groups converted to PPO plans through its Uniprise business group.
Companies like Aetna Health and Humana are following a similar approach. They are much less interested in managing insurance risk and have focused their efforts on providing plan administration services, especially to large, multi-site, self-funded employers.
As Exhibit 2 showed, this combination of strategies led HMOs back to profitability. Even in Texas, HMOs ended 2002 at a breakeven point, a major swing from two straight years of losses of $500 million. In all of the other state, HMOs were profitable in the first two or three quarters of 2002. Thats the good news.
The not so good news is that HMOs are barely staying ahead of increased medical costs. Wall Street analysts look for the spread between premium revenues and medical spending and, while that has been healthy recently, it is under pressure.
Hospitals in particular have negotiated large payment increases and rates of utilization are climbing steadily. Add to that the expense of new drugs and medical technology and HMOs are faced with strong upward pressure on their medical expenses. Exhibit 3 uses a Minnesota illustration to show that medical spending PMPMs are increasing as fast as premiums, and in some years even faster. Minnesota HMOs had underwriting profits of $23 million in 2001 on their commercial lives. But in 2002 that fell to $3 million. The difference is found in the fact that premium revenues grew by 9.9% in 2002 while medical spending increased by more than 13%.
Exhibit 3: HMO Commercial Premium Revenue and Medical Spending in Minnesota, Per Member Per Month, 1997-2002

In 2001, for example, premium revenue of $190 PMPM exceeded medical spending by $7. But in 2002, Minnesota HMOs collected premium revenues of $209 PMPM and paid medical expenses of $208. Thats hardly any spread at all.
In summary, HMOs are profitable for now but are facing strong pressures on their spending. Because they are running into resistance on their premium increases, they are shifting more of the costs to consumers in the form of co-payments and deductibles. The outlook for the future is mixed they may enjoy a few years of profits, but the forces that are driving medical costs up continue unabated. And that will make it harder for them to balance profits and premiums in the future.